- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
C-Reactive Protein: A Prognostic Biomarker for ALS?
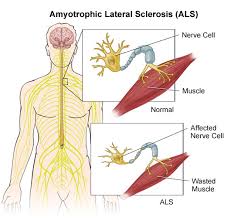
Serum levels of C-reactive protein (CRP) appear to be a "useful, feasible, and potentially prognostic factor" in patients with amyotrophic lateral sclerosis (ALS), a new study has suggested.
The authors also note that high CRP levels may identify patients with ALS who respond better to a new drug in development for the condition.
The findings were published online in JAMA Neurology on April 3, by a group led by Christian Lunetta, MD, Neuro Muscular Omnicentre, Fondazione Serena Onlus, Milan, Italy.
"CRP correlated very well with the severity of ALS in two different data sets," coauthor Stanley H. Appel, MD, chair for the Treatment and Research of ALS, Neurological Institute, Houston Methodist Hospital, Texas, commented to Medscape Medical News. "These showed that if patients are progressing faster, their CRP levels are higher. That is extremely interesting."
They explain that CRP is a biomarker of the inflammatory response with a significant prognostic value for several types of tumors, cardiovascular diseases, and rheumatic diseases.
They report that a recent phase 2 clinical trial of a novel immune regulator, NP001 (Neuraltus Pharmaceuticals), a pH-adjusted intravenous formulation of purified sodium chlorite that regulates inflammation, showed no significant benefit in the overall ALS population included but suggested that patients with high CRP levels treated with the drug had a slower progression of ALS than those receiving placebo.
Noting that a previous small study has shown a significant correlation between clinical disability in ALS and some sensitive biomarkers of inflammation, including CRP, they conducted new analyses to fully examine the prognostic significance of CRP in ALS.
For the analyses they evaluated serum CRP levels at first evaluation in a large cohort of patients with early-phase ALS from an Italian tertiary multidisciplinary center and in an independent cohort from a population-based registry of patients with ALS. Finally, they performed a post hoc analysis of the phase 2 trial of NP001 to evaluate whether CRP may help identify responders to the drug.
The Italian cohort included 394 patients with ALS. Results showed that serum CRP levels correlated with severity of functional impairment, as measured by total score on the ALS Functional Rating Scale Revised, at first evaluation (r = –0.14818; P = .004), and with patient survival.
The researchers report that "for every 1-point increase in the serum CRP level, we detected an effect of 13% on survival time" (hazard ratio, 1.129; 95% confidence interval [CI], 1.033 - 1.234).
Patients with elevated CRP, defined as above the median value (0.20 mg/dL), survived for an average of 19.79 months, compared with 22.79 months for those with lower CRP levels.
Use of the same CRP threshold as in the above studies in the post hoc analysis of the phase 2 trial of NP001 showed that patients with elevated baseline CRP levels receiving the higher dose of NP001 had significantly less functional impairment after the treatment period compared with patients with normal baseline CRP, regardless of whether patients with normal CRP levels received NP001 or placebo, the researchers report.

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd