- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
British Association of Dermatologists guidelines for the management of contact dermatitis 2017
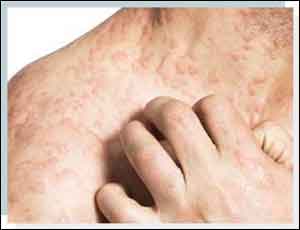
Contact dermatitis is a type of eczema triggered by contact with a particular substance.The prevalence of contact allergy is rising worldwide.In Europe about 20% of the general population suffers from contact allergy to at least one contact allergen. Most common are allergies to nickel, fragrances and preservatives.Contact dermatitis occurs twice as frequently in women as in men and often starts at a young age, with a prevalence of 15% in 12–16 year olds. British Association of Dermatologists' has issued guidelines for the management of contact dermatitis 2017, summary of which is as follows:
Summary of Recommendations
Diagnosis
Offer patients with suspected contact dermatitis a patch test with a baseline series of allergens. (Strong recommendation for the use of an intervention)
In identifying allergens in patients with contact dermatitis, consider testing for additional series dependent on allergen exposure. (Weak recommendation for the use of the intervention)
Consider additional readings at day 6 or 7 if the results are unexpectedly negative at day 4. (Weak recommendation for the use of the intervention)
Prevention
Consider skin care and skin protection creams in preventing occupational dermatitis. (Weak recommendation for the use of the intervention)
Treatment
Offer alitretinoin to patients with severe chronic hand eczema.* (Strong recommendation for the use of the intervention)
Consider topical tacrolimus to patients with contact dermatitis where topical steroids are unsuitable or ineffective. (Weak recommendation for the use of the intervention)
Consider psoralen plus ultraviolet A (PUVA) therapy for treating patients with chronic hand eczema. (Weak recommendation for the use of the intervention)
Consider patient education in occupational contact dermatitis. (Weak recommendation for the use of the intervention)
Summary of Good-Practice Recommendations (Informal Consensus)
Use clinical assessment tools such as the Dermatology Life Quality Index and the Hand Eczema Severity Index for both the initial assessment and the response to treatment of patients with contact dermatitis.
Take a detailed history, including symptoms and if they were related to application or use of any particular product, a specific activity or occupation.
If related to the workplace investigate the work practice and products handled at work, supplemented by examination of health and safety data sheets.
Provide a patient information leaflet on patch testing as part of the counselling process, which includes information on potential side-effects. Informed patient consent should be obtained.
Offer patch testing for patients with chronic or persistent dermatitis as clinical features alone are unreliable in distinguishing allergic contact from irritant and endogenous dermatitis, particularly with hand and facial dermatitis.
Consider deferring patch testing for 3 months after finishing systemic agents and 6 months after finishing biological agents to minimize the chance of false-negative reactions, if possible.
For more details click on the following link :
http://www.bad.org.uk/shared/get-file.ashx?id=4375&itemtype=document

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd