- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
Branchial Cyst - Standard Treatment Guidelines
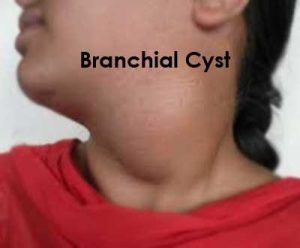
Branchial cleft cysts are congenital epithelial cysts, which arise on the lateral part of the neck from a failure of obliteration of the second branchial cleft in embryonic development. Phylogenetically, the branchial apparatus is related to gill slits. (Branchia is Greek for gills).
Ministry of Health and Family Welfare, Government of India has issued the Standard Treatment Guidelines for Branchial Cyst. Following are the major recommendations:
Definition:
At the fourth week of embryonic life, the development of 4 branchial (or pharyngeal) clefts results in 5 ridges known as the branchial (or pharyngeal) arches, which contribute to the formation of various structures of the head, the neck, and the thorax. The second arch grows caudally and, ultimately, covers the third and fourth arches. The buried clefts become ectoderm-lined cavities, which normally involutes around week 7 of development. If a portion of the cleft fails to involute completely, the entrapped remnant forms an epithelium-lined cyst with or without a sinus tract to the overlying skin.
Incidence in India:
Unknown. Branchial cleft cysts are the most common congenital cause of a neck mass. An estimated 2-3% of cases are bilateral. A tendency exists for cases to cluster in families.
Differential Diagnosis:
1. Lymphadenopathy (reactive, neoplastic, lymphoma, metastasis)
2. Vascular neoplasms and malformations
3. Capillary hemangioma
4. Carotid body tumor
5. Lymphatic malformation (cystic hygroma)
6. Ectopic thyroid tissue
7. Ectopic salivary tissue
Prevention and Counseling: NA
Optimal Diagnostic Criteria, Investigations, Treatment & Referral Criteria
Clinical Diagnosis:
Diagnosis is usually made clinically. Many branchial cleft cysts are asymptomatic. Depending on the size and the anatomical extension of the mass, local symptoms, such as neck swelling, dysphagia, dysphonia, dyspnea, and stridor may occur.
A branchial cyst commonly presents as a solitary, painless mass in the neck of a child or a young adult. A history of intermittent swelling and tenderness of the lesion during upper respiratory tract infection may exist. Discharge may be reported if the lesion is associated with a sinus tract.
Branchial cysts are smooth, non-tender, fluctuant, translucent masses, which occur along the lower one third of the antero-medial border of the sternocleidomastoid muscle between the muscle and the overlying skin.
Secondary branchial cleft cyst lesion: The lesion may be tender if secondarily inflamed or infected. When associated with a sinus tract, mucoid or purulent discharge onto the skin or into the pharynx may be present.
Investigations:
1. Fine-needle aspiration may be helpful to distinguish branchial cleft cysts from malignant neck masses. Fine-needle aspiration and culture may help guide antibiotic therapy for infected cysts.
2. A sinogram may be obtained. If a sinus tract exists, radio-opaque dye can be injected to delineate the course and to examine the size of the cyst.
3. Ultrasonography helps to delineate the cystic nature of these lesions.
4. A contrast-enhanced CT scan shows a cystic and enhancing mass in the neck. It may aid preoperative planning and identify compromise of local structures.
5. MRI allows for finer resolution during preoperative planning. The wall may be enhancing on gadolinium scans.
Treatment:
Surgical excision is definitive treatment for branchial cleft cysts. A series of horizontal incisions, known as a stair step or stepladder incision, is made to fully dissect out the occasionally tortuous path of the branchial cleft cysts.
Standard Operating Procedure : As in patient surgery should be performed
Referral Criteria:
depends upon competency of operating surgeon and available resources.
Guidelines by The Ministry of Health and Family Welfare :
Dr J M Hans Ex-HOD Dept. of Otorhinolaryngology Dr.RML Hospital New Delhi

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd