- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
AUA's New Guideline on Surgical Management of BPH related LUTS
The American Urological Association (AUA) has issued a new clinical practice guideline on the surgical management of lower urinary tract symptoms (LUTS) associated with benign prostatic hyperplasia (BPH). The guideline was published in the Journal of Urology. The American Urological Association (AUA) Guideline for the Management of Benign Prostatic Hyperplasia was last revised in 2010.
This new clinical guideline offers a framework to guide as to which surgical treatments are appropriate for treating BPH. In the guideline, the AUA expert panel encourages a shared decision-making process as the basis for choosing the most appropriate care for patients.
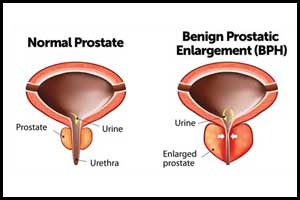
Benign prostatic hyperplasia also called prostate gland enlargement is a common condition in ageing males. An enlarged prostate gland can cause uncomfortable urinary symptoms, such as blocking the flow of urine out of the bladder. It can also cause bladder, urinary tract or kidney problems
The LUTS/BPH Panel was created in 2016 by the American Urological Association Education and Research, Inc.
There are 22 key recommendations including different parameters
Evaluation and Preoperative Testing
- Clinicians should take a medical history and utilize the AUA-Symptom Index (AUA-SI) and urinalysis in the initial evaluation of patients presenting with bothersome LUTS possibly attributed to Benign prostatic hyperplasia (Clinical Principle)
- Clinicians should consider the assessment of the prostate size and shape via abdominal or transrectal ultrasound, or cystoscopy, or by preexisting cross-sectional imaging (i.e. magnetic resonance imaging [MRI]/ computed tomography [CT]) prior to surgical intervention for LUTS attributed to Benign prostatic hyperplasia. (Clinical Principle)
- Clinicians should perform a PVR assessment prior to surgical intervention for LUTS attributed to Benign prostatic hyperplasia. (Clinical Principle)
- Clinicians should consider uroflowmetry prior to surgical intervention for LUTS attributed to Benign prostatic hyperplasia. (Clinical Principle)
- Clinicians should consider pressure flow studies prior to surgical intervention for LUTS attributed to BPH when diagnostic uncertainty exists. (Expert Opinion)
Surgical Therapy
- Surgery is recommended for patients who have renal insufficiency secondary to BPH, refractory urinary retention secondary to Benign prostatic hyperplasia, recurrent urinary tract infections (UTIs), recurrent bladder stones or gross hematuria due to Benign prostatic hyperplasia, and/or with LUTS attributed to BPH refractory to and/or unwilling to use other therapies. (Clinical Principle)
- Clinicians should not perform surgery solely for the presence of an asymptomatic bladder diverticulum; however, evaluation for the presence of BOO should be considered. (Clinical Principle)
Transurethral Resection of the Prostate (TURP)
- TURP should be offered as a treatment option for men with LUTS attributed to Benign prostatic hyperplasia. (Moderate Recommendation; Evidence Level: Grade B)
- Clinicians may use a monopolar or bipolar approach to TURP, depending on their expertise with these techniques. (Expert Opinion)
Simple Prostatectomy
- Clinicians should consider open, laparoscopic or robotic-assisted prostatectomy, depending on their expertise with these techniques, for patients with large prostates. (Moderate Recommendation; Evidence Level: Grade C)
Transurethral Incision of the Prostate (TUIP)
- TUIP should be offered as an option for patients with prostates ≤30g for the surgical treatment of LUTS attributed to BPH. (Moderate Recommendation; Evidence Level: Grade B)
Transurethral Vaporization of the Prostate (TUVP)
- Bipolar TUVP may be offered to patients for the treatment of LUTS attributed to benign prostatic hyperplasia. (Conditional Recommendation; Evidence Level: Grade B)
Photoselective Vaporization of the Prostate (PVP)
- Clinicians should consider PVP as an option using 120W or 180W platforms for patients for the treatment of LUTS attributed to BPH. (Moderate Recommendation; Evidence Level: Grade B)
Prostatic Urethral Lift (PUL)
- Clinicians should consider PUL as an option for patients with LUTS attributed to BPH provided prostate volume <80g and verified the absence of an obstructive middle lobe (Moderate Recommendation; Evidence Level: Grade C)
- PUL may be offered to eligible patients concerned with an erectile and ejaculatory function for the treatment of with LUTS attributed to Benign prostatic hyperplasia. (Conditional Recommendation; Evidence Level: Grade C)
Transurethral Microwave Therapy (TUMT)
- TUMT may be offered to patients with LUTS attributed to BPH; however, patients should be informed that surgical retreatment rates are higher compared to TURP. (Conditional Recommendation; Evidence Level: Grade C)
Water Vapor Thermal Therapy
- Water vapour thermal therapy may be offered to patients with LUTS attributed to Benign prostatic hyperplasia provided prostate volume <80g. (Conditional Recommendation; Evidence Level: Grade C)
- Water vapour thermal therapy may be offered to eligible patients who desire preservation of erectile and ejaculatory function. (Conditional Recommendation; Evidence Level: Grade C)
Transurethral Needle Ablation (TUNA)
- TUNA is not recommended for the treatment of LUTS attributed to Benign prostatic hyperplasia. (Expert Opinion)
Laser Enucleation
- Clinicians should consider holmium laser enucleation of the prostate (HoLEP) or thulium laser enucleation of the prostate (ThuLEP), depending on their expertise with either technique, as prostate size-independent suitable options for the treatment of LUTS attributed to Benign prostatic hyperplasia. (Moderate Recommendation; Evidence Level: Grade B)
Prostate Artery Embolization (PAE)
- PAE is not recommended for the treatment of LUTS attributed to BPH outside the context of a clinical trial. (Expert Opinion)
Medically Complicated Patients
- HoLEP, PVP, and ThuLEP should be considered in patients who are at higher risk of bleeding, such as those on anti-coagulation drugs. (Expert Opinion)
The guideline will help facilitate shared decision-making and guidance as to which surgical treatments are appropriate for treating BPH.
For more reference log on to:
https://www.auanet.org/guidelines/surgical-management-of-lower-urinary-tract-symptoms-attributed-to-benign-prostatic-hyperplasia-(2018)

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd