- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
AI better than experts at detecting Retinopathy of prematurity
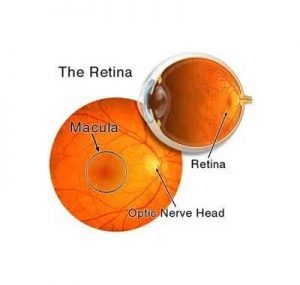
Retinopathy of prematurity is caused by abnormal blood vessel growth near the retina, the light-sensitive portion in the back of an eye and is the leading cause of childhood blindness globally.An algorithm that uses artificial intelligence can automatically and more accurately diagnose Retinopathy of prematurity than most expert physicians, a paper published in JAMA Ophthalmology suggests.
The algorithm accurately diagnosed the condition in images of infant eyes 91 percent of the time. On the other hand, a team of eight physicians with ROP expertise who examined the same images had an average accuracy rate of 82 percent.
"There's a huge shortage of ophthalmologists who are trained and willing to diagnose ROP. This creates enormous gaps in care, even in the United States, and sadly leads too many children around the world to go undiagnosed," said the study's co-lead researcher, Michael Chiang, M.D., a professor of ophthalmology and medical informatics & clinical epidemiology in the OHSU School of Medicine and a pediatric ophthalmologist at the Elks Children's Eye Clinic in the OHSU Casey Eye Institute.
"This algorithm distills the knowledge of ophthalmologists who are skilled at identifying ROP and puts it into a mathematical model so clinicians who may not have that same wealth of experience can still help babies receive a timely, accurate diagnosis," said the other lead researcher, Jayashree Kalpathy-Cramer, Ph.D., of the Athinoula A. Martinos Center for Biomedical Imaging at Massachusetts General Hospital, who is also an associate professor of radiology at Harvard Medical School.
Leading cause of childhood blindness
The National Eye Institute of the National Institutes of Health reports that up to 16,000 U.S. babies experience retinopathy of prematurity to some degree, but only up to 600 become legally blind each year as a result. The condition is becoming more common as medical care for premature babies improves.
The disease is diagnosed by visually inspecting a baby's eye. Physicians typically use a magnifying device that shines light into a baby's dilated eye, but that approach can lead to variable and subjective diagnoses.
Computational smarts
Artificial intelligence, also called AI, enables machines to think like humans and is a growing field in health care. Last month, the FDA approved an AI device that detects diabetes-related eye disease. Others have tried developing computerized systems to diagnose retinopathy of prematurity, but none have been able to match the accuracy of visual diagnosis by physicians.
This algorithm specifically uses deep learning, a form of AI that mimics how humans perceive the world through vision, including identifying objects. The MGH researchers combined two existing AI models to create the algorithm, while the OHSU researchers developed extensive reference standards to train it.
They first trained the algorithm to identify retinal vessels in more than 5,000 pictures taken during infant visits to an ophthalmologist. Next, they trained it to differentiate between healthy and diseased vessels. Afterward, they compared the algorithm's accuracy with that of trained experts who viewed the same images and discovered it performed better than most of the expert physicians.
The full research team is now working with a collaborator in India to see if the algorithm can diagnose ROP in Indian babies as well as it did for the group of primarily Caucasian babies involved in this study. They are also exploring whether the algorithm can diagnose the condition in images of other parts of the retina besides vessels. The ultimate goal is to enable physicians to incorporate the technology into their clinical practices.
For more details click on the link: http://dx.doi.org/10.1001/jamaophthalmol.2018.1934

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd