- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
AHA Clinical Practice Guidelines for adults with Congenital Heart Disease
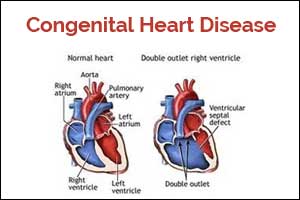
The American College of Cardiology/American Heart Association has released Clinical Practice Guidelines for the management of Adults With Congenital Heart Disease (ACHD).
The guidelines are published in the Journal of the American College of Cardiology.
Key Recommendations:
- A standard 12-lead ECG is recommended in adults with congenital heart disease (CHD) with serial assessment, depending on the adult CHD (ACHD) anatomic and physiologic (AP) classification or when symptoms develop or worsen.
- Ambulatory ECG monitoring should be performed in patients with CHD at risk of tachyarrhythmia, bradyarrhythmia, or heart block.
- Intraoperative transesophageal echocardiography (TEE) is recommended to guide the surgical repair of CHD.
- Patients with ACHD should undergo transthoracic echocardiography (TTE) for initial assessment.
- In patients with ACHD who have or are at risk of RV enlargement and dysfunction, serial cardiovascular magnetic resonance (CMR) is recommended.
- Patients with ACHD should be evaluated for depression and anxiety.
- Patients with ACHD at risk for hepatitis C should be screened and vaccinated for viral hepatitis.
- Patients at high risk of maternal morbidity or mortality, including women with pulmonary arterial hypertension (PAH), Eisenmenger syndrome, severe systemic ventricular dysfunction, severe left-sided obstructive lesions, and/or ACHD AP classification ID, IID, IIID should be counseled against becoming pregnant or be given the option of terminating a pregnancy.
- When either parent has CHD, it is reasonable to perform fetal echocardiography.
- Estrogen-containing contraceptives are potentially harmful to women with CHD who are at high risk of thromboembolic events such as cyanosis, Fontan physiology, mechanical valves, prior thrombotic events, and PAH.
- Pulse oximetry at rest and during exercise is recommended for evaluation of adults with unrepaired or repaired atrial septal defect (ASD) with the residual shunt.
- Adults with primum ASD, sinus venosus defect, or coronary sinus defect causing impaired functional capacity, right atrial and/or RV enlargement, and net left-to-right shunt resulting in physiologic sequelae (eg, Qp:Qs ≥1.5:1) without cyanosis at rest or during exercise should be surgically repaired unless precluded by comorbidities, provided that systolic PA pressure is less than 50% of systemic pressure and pulmonary vascular resistance is less than one third of systemic vascular resistance.
- ASD closure should not be performed in adults with PA systolic pressure greater than two thirds systemic, pulmonary vascular resistance greater than two thirds systemic, and/or a net right-to-left shunt.
- CMR or CT angiography (CTA) is recommended for evaluation of partial anomalous pulmonary venous connection.
- Repair of partial anomalous pulmonary venous connection is recommended at the time of closure of a sinus venosus defect or ASD.
- Adults with a ventricular septal defect (VSD) and evidence of left ventricular volume overload and hemodynamically significant shunts (Qp: Qs ≥1.5:1) should undergo VSD closure if PA systolic pressure is less than 50% systemic and pulmonary vascular resistance is less than one-third systemic.
- VSD closure should not be performed in adults with severe PAH with PA systolic pressure greater than two thirds systemic, pulmonary vascular resistance greater than two thirds systemic, and/or a net right-to-left shunt.
- Surgery for primary repair of atrioventricular septal defect or closure of residual shunts in adults with repaired atrioventricular septal defect is recommended when there is a net left-to-right shunt (Qp: Qs ≥1.5:1), a PA systolic pressure less than 50% systemic, and pulmonary vascular resistance less than one-third systemic.
- Surgery for primary repair of atrioventricular septal defect or closure of residual shunts in adults with repaired atrioventricular septal defect should not be performed when PA systolic pressure is greater than two thirds systemic, pulmonary vascular resistance is greater than two thirds systemic, or there is a presence of a net right-to-left shunt.
- Oxygen saturation should be measured in feet and hands in adults with a patent ductus arteriosus (PDA) to identify right-to-left shunting.
- PDA closure is recommended in adults if left atrial or LV enlargement is present and is attributed to PDA with net left-to-right shunt, PA systolic pressure that is less than 50% systemic, and pulmonary vascular resistance that is less than one-third systemic.
- Aortic imaging using TTE, TEE, CMR, or CTA is recommended in adults with Williams syndrome or patients suspected of having supravalvular aortic stenosis.
- Surgical repair is recommended for adults with supravalvular aortic stenosis (discrete or diffuse) and symptoms or decreased LV systolic function deemed secondary to aortic obstruction.
- Resting blood pressure should be measured in upper and lower extremities in all adults with coarctation of the aorta.
- Surgical repair or catheter-based stenting is recommended for adults with hypertension and significant native or recurrent coarctation of the aorta.
- Surgical or percutaneous pulmonary valve replacement for the relief of symptoms is recommended for patients with repaired tetralogy of Fallot and moderate or greater PR with cardiovascular symptoms that cannot be otherwise explained.
- Cardiac catheterization to assess pulmonary vascular hemodynamics is recommended for adults with septal or great artery shunts and clinical symptoms, signs, or ECG findings suggestive of pulmonary hypertension.
For further reference follow the link: 10.1016/j.jacc.2018.08.1029
cardiacCatheterizationComputed tomographycongenitalCTdiseaseductus arteriosusECGguidelinesHeartimagingJournal of the American College of Cardiologypatentpulmonary arterial hypertensionventricular septal defect
Source : With inputs from JACCNext Story
NO DATA FOUND

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd