- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
Acute Bacterial Rhinosinusitis- Guidelines 2016
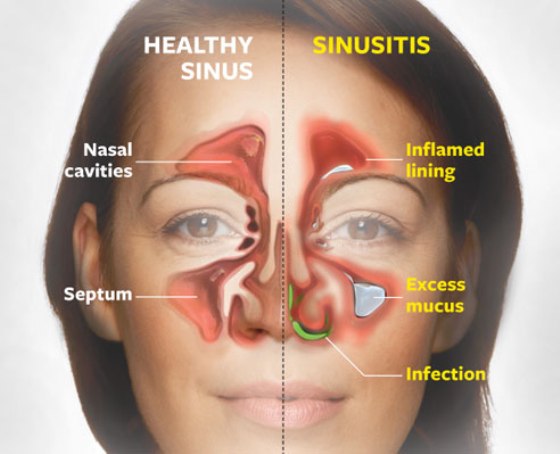
Most cases of acute Bacterial Rhinosinusitis, inflammation of the paranasal sinuses (sinusitis) is accompanied by inflammation of the nasal passages (rhinitis); thus the clinical condition often referred to as sinusitis is, in fact, rhino sinusitis: inflammation of the sinuses with concomitant inflammation of the nasal passages.
Despite the common nature of rhino sinusitis, its management is controversial. Therapies are usually directed to alleviating or reducing symptoms, eradicating the underlying cause, or both. A major question is whether an antibiotic should be used and, if so, which one? Because the premise of treatment with antibiotics is that bacterial infection will be eliminated, patients with bacterial rhino sinusitis need to be identified. In addition, other disease and patient characteristics, such as age and duration and pattern of illness, may help in distinguishing patient subgroups for more specific types of treatment (e.g., antibiotics to eradicate specific bacteria). Because bacterial infection of the sinuses is potentially serious, the use of antimicrobials to prevent complications is of interest. However, concern is increasing about the overuse or abuse of antibiotics, both for the individual-in terms of potential side effects and cost-as well as for society, in terms of cost and the development of antibiotic-resistant bacteria.
In the latest Clinical Practice Guideline for acute Bacterial Rhinosinusitis-2016, the IDSA ( Infectious Diseases Society of America) has published the following recommendations:
Initial Treatment
Recommendations
- The following clinical presentations (any of 3) are recommended for identifying patients with acute bacterial vs. viral rhinosinusitis:
- Onset with persistent symptoms or signs compatible with acute rhinosinusitis, lasting for ≥10 days without any evidence of clinical improvement (strong recommendation)
- Onset with severe symptoms or signs of high fever (≥39°C [102°F]) and purulent nasal discharge or facial pain lasting for at least 3–4 consecutive days at the beginning of illness (strong recommendation)
- Onset with worsening symptoms or signs characterized by the new onset of fever, headache, or increase in nasal discharge following a typical viral upper respiratory infection (URI) that lasted 5–6 days and were initially improving ("double sickening") (strong recommendation).
Recommendation
- It is recommended that empiric antimicrobial therapy be initiated as soon as the clinical diagnosis of ABRS is established as defined in recommendation 1 above (strong recommendation).
Recommendation
- Amoxicillin-clavulanate rather than amoxicillin alone is recommended as empiric antimicrobial therapy for ABRS in children(strong recommendation).
Recommendation
- Amoxicillin-clavulanate rather than amoxicillin alone is recommended as empiric antimicrobial therapy for ABRS in adults(weak recommendation).
Recommendation
- "High-dose" (2 g orally twice daily or 90 mg/kg/day orally twice daily) amoxicillin-clavulanate is recommended for children and adults with ABRS from geographic regions with high endemic rates (≥10%) of invasive penicillin-nonsusceptible (PNS)S. pneumoniae, those with severe infection (e.g., evidence of systemic toxicity with fever of 39°C [102°F] or higher, and threat of suppurative complications), attendance at daycare, age <2 or >65 years, recent hospitalization, antibiotic use within the past month, or who are immunocompromised (weak recommendation).
Recommendation
- A β-lactam agent (amoxicillin clavulanate) rather than a respiratory fluoroquinolone is recommended for initial empiric antimicrobial therapy of ABRS (weak recommendation).
Recommendations
- Macrolides (clarithromycin and azithromycin) are not recommended for empiric therapy due to high rates of resistance among S. pneumoniae (~30%) (strong recommendation).
- Trimethoprim-sulfamethoxazole (TMP/SMX) is not recommended for empiric therapy because of high rates of resistance among both S. pneumoniae and Haemophilus influenzae (~30%–40%) (strong recommendation).
- Doxycycline may be used as an alternative regimen to amoxicillin-clavulanate for initial empiric antimicrobial therapy of ABRS in adults because it remains highly active against respiratory pathogens and has excellent pharmacokinetic/pharmacodynamic (PK/PD) properties (weak recommendation).
- Second-and third-generation oral cephalosporins are no longer recommended for empiric monotherapy of ABRS due to variable rates of resistance among S. pneumoniae. Combination therapy with a third-generation oral cephalosporin (cefixime or cefpodoxime) plus clindamycin may be used as second-line therapy for children with non–type I penicillin allergy or from geographic regions with high endemic rates of PNS S. pneumoniae(weak recommendation).
Recommendations
- Either doxycycline (not suitable for children) or a respiratory fluoroquinolone (levofloxacin or moxifloxacin) is recommended as an alternative agent for empiric antimicrobial therapy in adults who are allergic to penicillin (strong recommendation).
- Levofloxacin is recommended for children with a history of type I hypersensitivity to penicillin; combination therapy with clindamycin plus a third-generation oral cephalosporin (cefixime or cefpodoxime) is recommended in children with a history of non–type I hypersensitivity to penicillin (weak recommendation).
Recommendation
- Although S. aureus (including methicillin-resistant S. aureus [MRSA]) is a potential pathogen in ABRS, on the basis of current data, routine antimicrobial coverage for S. aureus or MRSA during initial empiric therapy of ABRS is not recommended (strong recommendation).
Recommendations
- The recommended duration of therapy for uncomplicated ABRS in adults is 5–7 days (weak recommendation).
- In children with ABRS, the longer treatment duration of 10–14 days is still recommended (weak recommendation).
Recommendation
- Intranasal saline irrigation with either physiologic or hypertonic saline is recommended as an adjunctive treatment in adults with ABRS (weak recommendation).
Recommendation
- Intranasal corticosteroids (INCSs) are recommended as an adjunct to antibiotics in the empiric treatment of ABRS, primarily in patients with a history of allergic rhinitis (weak recommendation).
Recommendation
- Neither topical nor oral decongestants and/or antihistamines are recommended as adjunctive treatment in patients with ABRS (strong recommendation).
Nonresponsive Patient
Recommendation
- An alternative management strategy is recommended if symptoms worsen after 48–72 hours of initial empiric antimicrobial therapy or fail to improve despite 3–5 days of initial empiric antimicrobial therapy (strong recommendation).
Recommendation
- An algorithm for managing patients who fail to respond to initial empiric antimicrobial therapy is shown in Figure 1 in the original guideline document. Patients who clinically worsen despite 72 hours or fail to improve after 3–5 days of empiric antimicrobial therapy with a first-line agent should be evaluated for the possibility of resistant pathogens, a noninfectious etiology, structural abnormality, or other causes for treatment failure (strong recommendation).
Recommendations
- It is recommended that cultures be obtained by direct sinus aspiration rather than by nasopharyngeal swab in patients with suspected sinus infection who have failed to respond to empiric antimicrobial therapy (strong recommendation).
- Endoscopically guided cultures of the middle meatus may be considered as an alternative in adults, but their reliability in children has not been established (weak recommendation).
- Nasopharyngeal cultures are unreliable and are not recommended for the microbiologic diagnosis of ABRS (strong recommendation).
Recommendation
- In patients with ABRS suspected to have suppurative complications, axial and coronal views of contrast-enhanced computed tomography (CT) rather than magnetic resonance imaging (MRI) is recommended to localize the infection and to guide further treatment (weak recommendation).
Recommendation
- Patients who are seriously ill and immunocompromised, continue to deteriorate clinically despite extended courses of antimicrobial therapy, or have recurrent bouts of acute rhinosinusitis with clearing between episodes should be referred to a specialist (such as an otolaryngologist, infectious disease specialist, or allergist) for consultation. As this is a "good clinical practice" statement rather than a recommendation, it is not further graded
To read further click on the following Link :
http://cid.oxfordjournals.org/content/54/8/1041.long
Next Story
NO DATA FOUND

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd