- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
AAO-HNSF Clinical Practice Guidelines on Bell's Palsy
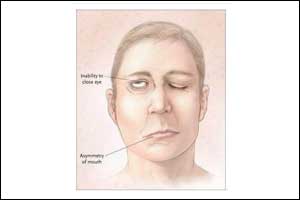
The American Academy of Otolaryngology-Head and Neck Surgery Foundation (AAO-HNSF) has published a supplement to this issue featuring the new Clinical Practice Guideline: Bell’s Palsy.The guideline is intended for clinicians in any setting who are likely to diagnose and manage patients with Bell’s palsy, the most common single nerve disorder, usually associated with facial paralysis.The purpose of the guideline is to improve the accuracy of diagnosis for Bell’s palsy, to improve the quality of care and outcomes for patients with Bell’s palsy, and to decrease harmful variations in the evaluation and management of Bell’s palsy.
Risk factors for Bell’s palsy include
- Pregnancy
- Severe preeclampsia
- Obesity
- Hypertension and chronic hypertension
- Diabetes
- Upper respiratory ailments
Main recommendations
1.Patient history and physical examination:
- Clinicians should assess the patient using history and physical examination to exclude identifiable causes of facial paresis or paralysis in patients presenting with acute onset unilateral facial paresis or paralysis.
2.Laboratory testing:
- Clinicians should not obtain routine laboratory testing in patients with new-onset Bell’s palsy
3.Diagnostic imaging:
- Clinicians should not routinely perform diagnostic imaging for patients with new-onset Bell’s palsy.
4.Oral steroids:
- Clinicians should be prescribed within 72 hours of symptom onset for Bell’s palsy patients 16 years and older.
5.Antiviral therapy:
- Monotherapy: Clinicians should not prescribe oral antiviral therapy alone for patients with new-onset Bell’s palsy.
- Combination antiviral therapy: Clinicians may offer oral antiviral therapy in addition to oral steroids within 72 hours of symptom onset for patients with Bell’s palsy.
6.Eye care:
- Clinicians should implement eye protection for Bell’s palsy patients with impaired eye closure.
7.Electrodiagnostic testing:
- In patients with incomplete paralysis: Clinicians should not perform electrodiagnostic testing in Bell’s palsy patients with incomplete facial paralysis.
- In patients with complete paralysis: Clinicians may offer electrodiagnostic testing to Bell’s palsy patients with complete facial paralysis.
8.Surgical decompression:
- No recommendation can be made regarding surgical decompression for Bell’s palsy patients.
9.Acupuncture:
- No recommendation can be made regarding the effect of acupuncture in Bell’s palsy patients.
10.Physical therapy:
- No recommendation can be made regarding the effect of physical therapy in Bell’s palsy patients.
11.Patient follow-up:
Clinicians should reassess or refer to a facial nerve specialist those Bell’s palsy patients with
- new or worsening neurologic findings at any point,
- ocular symptoms developing at any point, or
- incomplete facial recovery 3 months after initial symptom onset.
This guideline does not focus on facial paresis/paralysis due to neoplasms, trauma, congenital or syndromic problems, specific infectious agents, or postsurgical facial paresis or paralysis, nor does it address recurrent facial paresis/paralysis.
For more details click on the link: http://www.entnet.org/content/clinical-practice-guideline-bells-palsy

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd