- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
A rare case of Diabetes presenting with Quadriparesis
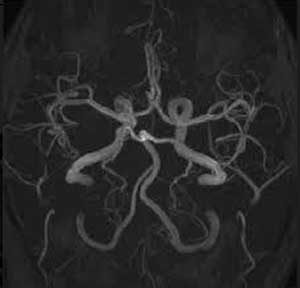
A rare case of Diabetic complication, Central pontine myelinolysis has been reported which has appeared in the Indian Journal of Endocrinology and Metabolism. Central pontine myelinolysis is a noninflammatory, demyelinating condition that has been described mostly in the context of rapid correction of hyponatremia. Classical clinical manifestations range from a depressed level of consciousness to dysarthria and flaccid quadriplegia.
According to history, a 50-year-old male patient presented with a history of slurring of speech, unsteadiness of gait, and weakness of the upper and lower limbs for the 10-day duration. There was no history of a headache, seizures, or altered sensorium. There were no sensory or bowel bladder symptoms. There was no history of fever, neck pain, or weight loss.
On examination, he was consciously oriented; fundus examination and extraocular movements were normal. He had emotional lability, dysarthria with bifacial weakness, mild dysphagia, and flaccid quadriparesis with Grade 3 power. There was no sensory level, spinal deformity, or tenderness.
Laboratory evaluation revealed random blood sugar 546 mg/dl, hemoglobin A1c 13%, serum creatinine 1.2 mg/dl, blood urea 66 mg/dl, and serum electrolytes such as sodium 135 mmol/L and potassium 3.6 mmol/L. Arterial-blood gas revealed normal pH and bicarbonate levels. Urine sugar 3 plus and ketones are negative. Measured serum osmolality was 318 mosm/kg.
Hemogram, erythrocyte sedimentation rate, liver function test, chest X-ray, ultrasonography abdomen, electrocardiograph, and two-dimensional echo were normal. Nerve conduction studies were normal. Pontine localization with possibilities of stroke or myelinolysis was considered.
MRI brain with MR angiogram revealed T2 and fluid-attenuated inversion recovery hyperintensity in the central pons with sparing thin peripheral rim and showing diffusion restriction. MR angiogram was unremarkable. In the given clinical scenario, the imaging features were suggestive of pontine myelinolysis.
He was managed with intravenous insulin infusion, isotonic and half normal saline with close monitoring of blood sugar, urine output, and electrolytes. Supportive care, deep vein thrombosis prophylaxis, and physical rehabilitation were started simultaneously.
Over the next 10 days, the patient improved and was able to walk with minimal support, and by 1 month at follow-up, he was independent of all activities of daily living with mild dysarthria.
Central pontine myelinolysis is described in the context of hyponatremia correction, malnutrition, and alcoholism. Previous reports described association with hyperosmolar hyperglycemic status; however, presentation in de novo diabetic patient as in our case is very rare.
As our patient had undergone MRI brain within 2 h of presentation, the observed radiological abnormalities, which conformed to the clinical presentation, were believed to be the result of the patient's hyperglycemic hyperosmolar state and not secondary to the treatment of the same.
Saini et al. described the subacute presentation of ataxia and pseudobulbar palsy in a known diabetic patient as a manifestation of osmotic demyelination. Central pontine myelinolysis can also occur in the hyperglycemic hyperosmolar state with consistently normal serum sodium. Osmotic demyelination syndrome as the initial manifestation of a hyperosmolar hyperglycemic state was also described.
CPM is associated with the destruction of myelin in the center of basis pontis. Pathophysiologically, it is caused by sudden shrinkage of brain cells, oligodendrocytes in particular, and demyelination due to rapid change in the serum osmolality. Disruption of the blood-brain barrier and oligodendrocyte apoptosis are postulated. The axons are largely preserved. Having great admixture of white matter tracts and gray matter might be the reason for pontine predilection. Treatment is mainly supportive and addressing the comorbidities. The outcome may range from full recovery to permanent dependency/death.
This case highlights a rare complication of undiagnosed or untreated diabetes mellitus with normal serum sodium. Hyperglycemia evaluation should be included in all cases of pontine myelinolysis irrespective of alternative etiology.
For more details click on the link: DOI: 10.4103/ijem.IJEM_110_18

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd