- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
A case of disseminated histoplasmosis in patient with HIV infection: NEJM
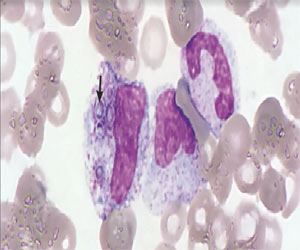
A case report published in the New England Journal of Medicine presents the case of a 30-year-old man with human immunodeficiency virus (HIV) infection presented to the emergency department with a 2-week history of fever, bloody diarrhea, and generalized weakness. He had discontinued antiretroviral therapy 3 months before presentation and then had spent 2 months in French Guiana. On physical examination, the patient was febrile, pale, and cachectic. Laboratory findings showed pancytopenia, a CD4+ cell count of 6 per cubic millimeter, and a C-reactive protein level of 239 mg per liter (reference range, 0 to 5).
Giemsa staining of a peripheral-blood sample revealed numerous myeloid cells containing intracytoplasmic yeast-like forms (arrow), a finding consistent with Histoplasma capsulatum.
Disseminated histoplasmosis is an opportunistic infection; when it occurs in patients with HIV infection, it is typically seen in those with a CD4+ cell count of less than 150 per cubic millimeter.
The patient was started on liposomal amphotericin B. His hospital course was complicated by hematemesis, and he died from complications of gastrointestinal hemorrhage. The diagnosis of disseminated histoplasmosis was confirmed with a positive result for H. capsulatum in peripheral blood and bone marrow aspirate on polymerase-chain-reaction analysis.
For more details click on the link: DOI: 10.1056/NEJMicm1809792

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd