- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
Guideline for reversal of antithrombotics in intracranial hemorrhage
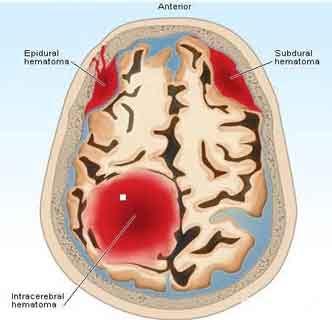
The use of antithrombotic agents, including anticoagulants, antiplatelet agents, and thrombolytics has increased over the last decade and is expected to continue to rise. Although antithrombotic-associated intracranial hemorrhage can be devastating, rapid reversal of coagulopathy may help limit hematoma expansion and improve outcomes.
In Feb 2016, Neurocritical Care Society and Society of Critical Care Medicine issued guidelines on reversal of antithrombotics in intracranial hemorrhage. Following are its major recommendations
Recommendations for Vitamin K Antagonists (VKA) Reversal
- The authors recommend discontinuing VKAs when intracranial hemorrhage is present or suspected. (Good Practice statement)
- The authors recommend urgent reversal of VKAs in patients with intracranial hemorrhage (Strong recommendation, moderate-quality evidence) with the following considerations:
- The authors suggest against VKA reversal in patients where there is a high suspicion of intracranial hemorrhage due to cerebral venous thrombosis. (Conditional recommendation, very low-quality evidence)
- The authors recommend assessing risks and benefits when considering VKA reversal in intracranial hemorrhage patients with concurrent symptomatic or life-threatening thrombosis, ischemia, heparin-induced thrombocytopenia, or disseminated intravascular coagulopathy (DIC). (Good Practice statement)
- The authors recommend administration of vitamin K to ensure durable reversal of international normalizing ratio (INR) following VKA-associated intracranial hemorrhage. Vitamin K should be dosed as soon as possible or concomitantly with other reversal agents. (Strong recommendation, moderate-quality evidence)
- The authors suggest one dose of vitamin K 10 mg intravenous [IV]). Subsequent treatment should be guided by follow-up INR. (Good Practice statement)
- If repeat INR is still elevated ≥1.4 within the first 24 to 48 h after reversal agent administration, the authors suggest redosing with vitamin K 10 mg IV. (Good Practice statement)
- The authors recommend administering 3-factor or 4-factor prothrombin complex concentrates (PCC) rather than fresh frozen plasma (FFP) to patients with VKA-associated intracranial hemorrhage and INR ≥1.4. (Strong recommendation, moderate-quality evidence)
- The authors suggest the use of 4-factor PCC over 3-factor PCC. (Conditional recommendation, low-quality evidence)
- The authors suggest initial reversal with PCC alone (either 3- or 4-factor) rather than combined with FFP or recombinant factor VIIa (rFVIIa). (Conditional recommendation, low-quality evidence)
- The authors recommend that PCC dosing should be weight-based and vary according to admission INR and type of PCC used. (Strong recommendation, moderate-quality evidence)
- The authors recommend repeating INR testing soon after PCC administration (15–60 min), and serially every 6 to 8 h for the next 24 to 48 h. Subsequent treatment should be guided by follow-up INR, with consideration given to the fact that repeat PCC dosing may lead to increased thrombotic complications and risk of DIC. (Good Practice statement)
- If the repeat INR is still elevated ≥1.4 within the first 24–48 h after initial PCC dosing, the authors suggest further correction with FFP. (Conditional recommendation, low-quality evidence)
- The authors recommend against administration of rFVIIa for the reversal of VKA. (Strong recommendation, low-quality evidence)
- If PCCs are not available or contraindicated, alternative treatment is recommended over no treatment. (Strong recommendation, moderate-quality evidence) Treatment choice may be guided by available therapies and patient-specific factors. (Good Practice statement)
- Treatment with FFP and vitamin K is recommended over no treatment. (Strong recommendation, moderate-quality evidence)
- The authors suggest dosing FFP at 10–15 ml/kg IV along with one dose of vitamin K 10 mg IV. (Conditional recommendation, low-quality evidence)
Recommendations for Oral Direct Factor Xa Inhibitors Reversal
- The authors recommend discontinuing factor Xa inhibitors when intracranial hemorrhage is present or suspected. (Good Practice statement)
- The authors recommend obtaining information on the time elapsed since the last dose of direct factor Xa inhibitor and possible medication interactions to assist in estimating the degree of anticoagulation exposure. (Good Practice statement)
- The authors suggest that pharmacological reversal of oral factor Xa inhibitors should be guided primarily by bleeding (major or intracranial) and not primarily by laboratory testing. (Conditional recommendation, low-quality evidence)
- The authors suggest administration of activated charcoal (50 g) to intubated intracranial hemorrhage patients with enteral access and/or those at low risk of aspiration who present within 2 h of ingestion of an oral direct factor Xa inhibitor. (Conditional recommendation, very low-quality evidence)
- The authors suggest administering a 4-factor PCC (50 units/kg) or activated PCC (aPCC) (50 units/kg) if intracranial hemorrhage occurred within 3 to 5 terminal half-lives of drug exposure or in the context of liver failure. (Conditional recommendation, low-quality evidence)
- The authors suggest administering 4-factor PCC or aPCC over rFVIIa because of the lower risk of adverse thrombotic events. (Conditional recommendation, low-quality evidence)
Recommendations for Direct Thrombin Inhibitor (DTI) Reversal
- The authors recommend discontinuing direct thrombin inhibitors when intracranial hemorrhage is present or suspected. (Good Practice statement)
- The authors recommend assessing the time and amount of the last ingested dose, renal function, and possible medication interactions to assist in estimating the degree of anticoagulation exposure. (Good Practice statement)
- The authors suggest that pharmacological reversal of direct thrombin inhibitors should be guided primarily by bleeding (major or intracranial) and not primarily by laboratory testing. (Conditional recommendation, low-quality evidence)
- The authors suggest administering activated charcoal (50 g) to intubated intracranial hemorrhage patients with enteral access and/or those at low risk of aspiration who present within 2 h of ingestion of an oral direct thrombin inhibitor. (Conditional recommendation, very low-quality evidence)
- The authors recommend administering idarucizumab (5 g IV in two divided doses) to patients with intracranial hemorrhage associated with dabigatran if:
- The dabigatran was administered within a period of 3 to 5 half-lives and there is no evidence of renal failure (Strong recommendation, moderate-quality of evidence) or
- There is renal insufficiency leading to continued drug exposure beyond the normal 3 to 5 half-lives (Strong recommendation, moderate-quality of evidence)
- The authors suggest administering aPCC (50 units/kg) or 4-factor PCC (50 units/kg) to patients with intracranial hemorrhage associated with direct thrombin inhibitors if idarucizumab is not available or if the hemorrhage is associated with a DTI other than dabigatran if:
- The direct thrombin inhibitor was administered within a period of 3 to 5 half-lives and there is no evidence of renal failure (Conditional recommendation, low-quality evidence) or
- There is renal insufficiency leading to continued drug exposure beyond the normal 3 to 5 half-lives. (Conditional recommendation, low-quality evidence)
- In patients with dabigatran-associated intracranial hemorrhage and renal insufficiency or dabigatran overdose, the authors suggest hemodialysis if idarucizumab is not available. (Conditional recommendation, low-quality evidence)
- In patients with dabigatran-associated intracranial hemorrhage who have already been treated with idarucizumab, PCC, or aPCC, with ongoing evidence of clinically significant bleeding, the authors suggest consideration of redosing idarucizumab and/or hemodialysis. (Conditional recommendation, low-quality evidence)
- The authors recommend against administration of rFVIIa or FFP in direct thrombin inhibitor-related intracranial hemorrhage. (Strong recommendation, low-quality evidence)
Recommendations for Unfractionated Heparin (UHF) Reversal
- The authors recommend discontinuing heparin infusions when intracranial hemorrhage is present or suspected. (Good Practice statement)
- The authors recommend urgently reversing anticoagulation in patients who develop intracranial hemorrhage during full dose heparin infusion. (Good Practice statement)
- The authors do not recommend routinely reversing prophylactic subcutaneous heparin. (Good Practice statement)
- The authors suggest considering reversal of prophylactic subcutaneous heparin if the activated partial thromboplastin time (aPTT) is significantly prolonged. (Good Practice statement)
- The authors recommend administering intravenous protamine sulfate to reverse heparin in the context of intracranial hemorrhage. (Strong recommendation, moderate-quality evidence)
- The authors recommend dosing protamine according to the dose of heparin infused over the preceding 2 to 3 h. (Strong recommendation, high-quality evidence)
- The authors recommend dosing protamine sulfate at 1 mg for every 100 units of heparin given in the previous 2 to 3 h with a maximum single dose of 50 mg. (Strong recommendation, moderate-quality evidence)
- If the aPTT remains elevated, the authors suggest repeat administration of protamine at a dose of 0.5 mg protamine per 100 units of UFH. (Conditional recommendation, low quality of evidence)
Recommendations for Low-Molecular Weight Heparin (LMWH) Reversal
- The authors recommend discontinuing LMWH when intracranial hemorrhage is present or suspected. (Good Practice statement)
- The authors recommend reversing LMWH in patients with intracranial hemorrhage receiving therapeutic doses of LMWH. (Strong recommendation, moderate-quality evidence)
- The authors recommend protamine administration by slow intravenous injection over a period of about 10 min according to the following dosing:
- For enoxaparin: If enoxaparin was given within 8 h, protamine sulfate should be administered at a dose of 1 mg per 1 mg of enoxaparin administered (up to a maximum single dose of 50 mg). If enoxaparin was given within 8 to 12 h, a dose of 0.5 mg of protamine per 1 mg of enoxaparin should be administered. After 3 to 5 half-lives have elapsed, protamine is probably not needed. (Strong recommendation, moderate-quality evidence)
- For dalteparin, nadroparin, and tinzaparin: Dose protamine at 1 mg per 100 anti-Xa units of LMWH administered in the past 3 to 5 half-lives of the drug, up to a maximum single dose of 50 mg. (Strong recommendation, moderate-quality evidence)
- If life-threatening bleeding persists, or the patient has renal insufficiency, the authors suggest redosing protamine (0.5 mg of protamine per 100 anti-Xa units or per 1 mg of enoxaparin). (Conditional recommendation, very low-quality evidence)
- The authors suggest considering recombinant factor VIIa (90 mcg/kg IV) if protamine is contraindicated. (Conditional recommendation, very low-quality evidence)
- The authors recommend against the reversal of LMWH in patients with intracranial hemorrhage receiving prophylactic dosing of LMWH. (Good Practice statement).
- The authors suggest against reversing danaparoid with protamine. (Conditional recommendation, low-quality evidence)
- The authors suggest reversing danaparoid with recombinant factor VIIa (90 mcg/kg IV once) in the context of intracranial hemorrhage. (Conditional recommendation, very low-quality evidence)
- The authors suggest against using FFP, PCC, or aPCC to reverse LMWH. (Conditional recommendation, low-quality evidence)
Recommendations for Pentasaccharide Reversal
- The authors recommend discontinuing pentasaccharides when intracranial hemorrhage is present or suspected. (Good Practice statement)
- The authors suggest reversing pentasaccharides in patients with intracranial hemorrhage receiving full therapeutic doses. (Good Practice statement)
- The authors suggest administration of aPCC (20 units/kg) for reversal of pentasaccharides. (Conditional recommendation, low-quality evidence)
- If aPCC is contraindicated or not available, the authors suggest administration of rFVIIa (90 mcg/kg). (Conditional recommendation, low-quality evidence)
- The authors recommend against protamine for reversal of pentasaccharides. (Strong recommendation, low-quality evidence)
- In intracranial hemorrhage patients receiving pentasaccharides for venous thromboembolism prophylaxis, the authors suggest against reversal unless there is evidence of bioaccumulation or impaired clearance. (Good Practice statement)
Recommendations for Thrombolytic Reversal
- The authors recommend discontinuing thrombolytic agents when intracranial hemorrhage is present or suspected. (Good Practice statement)
- The authors suggest using cryoprecipitate (10 units initial dose) in patients with thrombolytic agent-related symptomatic intracranial hemorrhage who have received a thrombolytic agent in the previous 24 h. (Conditional recommendation, low-quality evidence)
- In cases where cryoprecipitate is contraindicated or not available in a timely manner, the authors suggest using an antifibrinolytic agent (tranexamic acid 10–15 mg/kg IV over 20 min or ε-aminocaproic acid 4–5 g IV) as an alternative to cryoprecipitate. (Conditional recommendation, very low-quality evidence)
- The authors suggest checking fibrinogen levels after administration of reversal agents. If the fibrinogen is less than 150 mg/dL, the authors suggest administration of additional cryoprecipitate. (Conditional recommendation, very low-quality evidence)
- It is unclear if platelet transfusion is useful and the authors cannot offer a recommendation at this time.
Recommendations for Antiplatelet Agent Reversal
- The authors recommend discontinuing antiplatelet agents when intracranial hemorrhage is present or suspected. (Good Practice statement)
- The authors suggest against platelet transfusion for patients with antiplatelet-associated intracranial hemorrhage who will not undergo a neurosurgical procedure, regardless of the type of platelet inhibitor, platelet function testing, hemorrhage volume, or neurological exam. (Conditional recommendation, low-quality evidence)
- The authors suggest platelet transfusion for patients with aspirin or adenosine diphosphate (ADP) inhibitor-associated intracranial hemorrhage who will undergo a neurosurgical procedure. (Conditional recommendation, moderate-quality of evidence)
- The authors recommend platelet function testing prior to platelet transfusion if possible. (Strong recommendation, moderate-quality evidence)
- When platelet function testing is not readily available, empiric platelet transfusion may be reasonable. (Conditional recommendation, low-quality evidence)
- The authors recommend against platelet transfusion for patients with laboratory documented platelet function within normal limits or documented antiplatelet resistance. (Strong recommendation, moderate-quality evidence)
- The authors suggest against platelet transfusion in nonsteroidal anti-inflammatory drugs (NSAIDs) or glycoprotein IIb/IIIa inhibitor-related intracranial hemorrhage, even in the context of neurosurgical intervention. (Conditional recommendation, very low-quality evidence)
- In candidates for platelet transfusion, the authors suggest an initial dose of one single-donor apheresis unit of platelets. Platelet testing is suggested prior to repeat platelet transfusion, if available and repeat transfusion should be used only for those with persistently abnormal platelet function tests and/or ongoing bleeding. (Conditional recommendation, moderate-quality evidence)
- The authors suggest consideration of a single dose of desmopressin (DDAVP) in intracranial hemorrhage (0.4 mcg/kg IV) associated with aspirin/cyclooxygenase-1 (COX-1) inhibitors or ADP receptor inhibitors. In patients deemed appropriate (e.g., those undergoing a neurosurgical procedure), DDAVP can be used in addition to platelet transfusion. (Conditional recommendation, low-quality evidence)
You can read the full Guideline by clicking on the following link :
- Frontera JA, Lewin JJ III, Rabinstein AA, Aisiku IP, Alexandrov AW, Cook AM, del Zoppo GJ, Kumar MA, Peerschke EI, Stiefel MF, Teitelbaum JS, Wartenberg KE, Zerfoss CL. Guideline for reversal of antithrombotics in intracranial hemorrhage: a statement for healthcare professionals from the Neurocritical Care Society and Society of Critical Care Medicine. Neurocrit Care. 2016 Feb;24(1):6-46. [434 references] PubMed
- http://www.neurocriticalcare.org/Portals/61/Docs/Guidelines/Coag/FINAL COPY COAG.pdf

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd